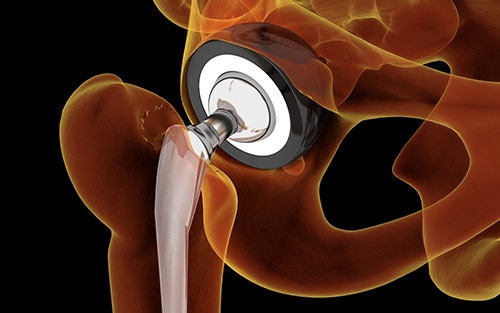
Hip Replacement Surgery and Recovery
Is your chronic hip pain disrupting your quality of life and mobility? Modern advancement in hip replacement surgery and recovery time may enable it to be the solution to your painful and inconvenient dilemma. yourfootpalace.com gathered detailed information about hip replacement surgery, the post-operation recovery process, and some of the forms of arthritis that lead … Read More