Do your feet hurt? That pain may represent a grave illness which can lead to severe debilitation or amputation if not addressed.
Our feet carry much more than our weight, they are responsible for our mobility and our physical stability. When something goes wrong with your feet, it should be addressed immediately before developing into something far more serious.
yourfootpalace.com gathered information on three common foot problems, their symptoms, and best treatment options.
Athlete’s Foot Symptoms and Treatment
Athlete’s foot, known as tinea pedis or ringworm of the foot, is a fungal infection affecting the feet. The fungus’ bacteria is easily transmitted from person to person by skin contact or any other contaminated surface. The infection typically appears first between the toes, and may spread like a rash to other parts of the feet, including infecting, thickening, and discoloring toenails.
Symptoms of Athlete’s Foot – The following symptoms may vary from person to person and in intensity:
• Itching, burning, stinging, peeling skin, or wounds between the toes
• Itchy rashes or blisters
• Dry, flaky skin on the soles or sides of your feet
• Cracking and peeling skin on the soles and heels
• Raw, itchy skin on your feet
• Discolored or deformed toenails
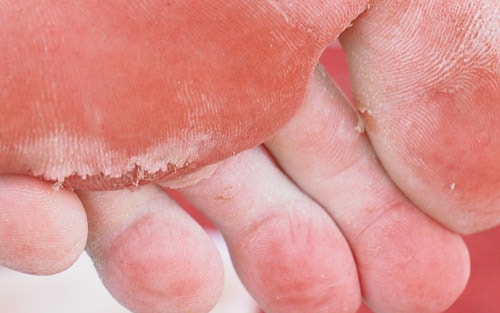
If you are experiencing any, or a combination of these symptoms, contact your primary care physician. Treating athlete’s foot may require medication and possible changes in hygiene. You may be referred to a podiatrist (foot doctor) or dermatologist (skin doctor). However, in most cases, your primary care physician can treat your infection successfully.
The following are used to treat athlete’s foot:
Topical Over The Counter (OTC) – Cremes, sprays, and ointments containing clotrimazole or terbinafine hydrochloride are effective in reversing the effects of athlete’s foot in its early stages.
Prescription Topical Medication – More severe cases of athlete’s foot may require more aggressive treatment. Your doctor may prescribe a topical medication containing:
• Ketoconazole
• Oxiconazole
• Sertaconazole
• Sulconazole
• Naftifine
• Clotrimazole
• Econazole
• Butenafine
• Ciclopirox
• Clotrimazole-betamethasone
Prescription Oral Medication – Prescription oral medication typically clears up infections much faster than topical applications. When necessary, the following oral medication may be prescribed:
• Terbinafine (Lamisil)
• Itraconazole (Sporanox)
While using oral anti-fungal drugs, there is a risk of developing hepatoxicity (chemical-driven liver damage) exacerbated by pre-existing liver disease, chemical components of the drug, drug to drug interactions, environmental factors, and patient demographics. Your doctor may occasionally request blood tests to evaluate and monitor the effects on your liver.
Plantar Fasciitis Symptoms and Treatment
The plantar fascia is a band of deep tissue running from the heel bone to the toes. Plantar fasciitis injuries typically result from overuse, commonly occurring from repetitive actions involving running or jumping. It may also be related to bad or abnormal foot mechanics, improper, or poorly fitting footwear.
Plantar Fasciitis Symptoms – Plantar fasciitis is the deformation or a tear of this tissue. It may cause the following:
• Irritation
• Inflammation
• Pain
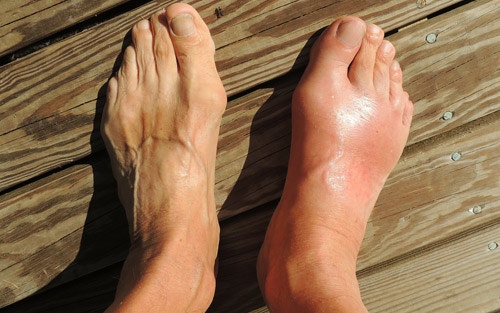
Some other factors that increase your risk of developing plantar fasciitis may include:
Age – Plantar fasciitis occurs more commonly in people between the ages of 30 and 60.
Obesity – Extra weight can stress the plantar fascia.
Standing – Long term standing on hard surfaces can damage the tissue.
The following treatment and tips may provide relief:
Wear Appropriate Footwear – Use footwear with a good fit, avoiding flat soles with little to no support.
Rest and Stretch – Rest is one key to recovery in cases of overuse. Combining that with daily stretching exercises and frequent massages will aid in the recovery process.
Use a Splint – A splint used at night can help keep your foot and ankle in the proper position while you sleep.
Ice Treatment – Roll your foot on a frozen water bottle for several minutes two to four times per day, or apply an ice pack to the bottom of your foot for 15 minutes, two to three times a day.
If the pain continues, consult your primary care physician.
For more on plantar fasciitis read yourfootpalace.com/how-foot-massage-can-relieve-your-plantar-fasciitis-pain/ and to schedule a foot massage, visit yourfootpalace.com
Diabetic Neuropathy Symptoms and Treatment
Nerve damage from diabetes is called diabetic neuropathy. Some form of nerve damage occurs in half of all those affected by diabetes.

Symptoms of Diabetic Neuropathy – The following symptoms may occur in those experiencing neuropathy:
• Lack of coordination, stumbling and falling
• Muscle weakness
• Numbness, prickling or tingling in the feet or hands
• Extreme sensitivity
• Pain during normal activities
• The sensation of wearing socks when you’re not
• Paralysis
• Heat intolerance
Treatment for Diabetic Neuropathy – Early treatment for those who already have nerve damage will help prevent or delay further damage:
• Keep your blood glucose levels on target
• Meal Planning
• Physical Activity
• Medication
The two ways to keep track of your blood glucose levels are:
• Use a blood glucose meter to guide you in adjusting your day-to-day care.
• Get an A1C test at least twice a year to reveal your average blood glucose for the past 2 to 3 months.
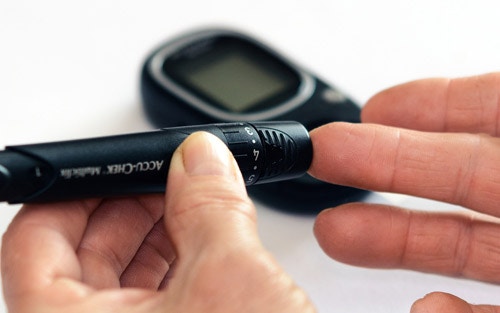
By checking your blood glucose levels regularly, you can detect whether your diabetes care plan is working or if changes may be needed. Make your feet a priority by:
• Paying attention to and taking care of your feet.
• Seeking immediate medical treatment if you experience heightening symptoms or problems.
• Using lotion on your skin for dry feet, and wear shoes and socks that fit well.
• Using warm water to wash your feet and drying them thoroughly.
• Checking your feet multiple times per day. A foot injury may go unnoticed if you are unable to feel pain. Injuries that become infected or left unattended may lead to severe health complications, including amputation.
• Special shoes may be required, and Medicare may pay for them. Ask your physician about this.
• Changes in your everyday routine may be required. Consult your physician on which exercises and activities should be avoided or altered to prevent foot injuries.

Use your eyes to inspect your feet, and use a mirror to see the bottoms of your feet. Using your hands, feel for bumps, and dry skin. Look for corns, calluses, blisters, swelling, ingrown toenails, and toenail infections. If you cannot see or reach your feet, get help from a friend, family member, or from your foot doctor.
For more detailed information about diabetic neuropathy, visit mayoclinic.org/diseases-conditions/peripheral-neuropathy/symptoms-causes/syc-20352061
Foot Pain and Common Problems
When your feet are hurting, don’t second guess it. Address it! When something goes wrong with your feet, treatment is usually simple and can be accomplished by making minor adjustments in your daily routine.
In this article, you discovered three common foot problems, their symptoms, and easy ways to treat them.
Ignoring your foot problems can lead to serious health risks, and when your foot pain is caused by a health problem, not treating it can lead to grave consequences.
Sources:
https://health.clevelandclinic.org/chronic-heel-pain-4-simple-fixes-for-your-plantar-fasciitis/
http://www.diabetes.org/living-with-diabetes/complications/neuropathy/
(706) 521-5290
(678) 963-5958